In clinical environments, the distinction between “clean” and “disinfected” is a matter of patient safety. Standard janitorial practices often fall short of the rigorous demands required to eliminate healthcare-associated infections (HAIs).
Professional medical cleaning services utilize evidence-based protocols to ensure that high-touch surfaces, waiting areas, and examination rooms meet stringent sanitation benchmarks.
These specialized processes are designed to mitigate the spread of pathogens like influenza, which can persist on surfaces for extended periods if not addressed with hospital-grade chemistry.
Understanding Regulatory Compliance and Safety Standards
Medical facilities must adhere to a complex web of regulations to maintain accreditation and ensure public health. Organizations such as the Centers for Disease Control and Prevention (CDC) provide exhaustive guidelines for environmental infection control.
Maintaining these standards requires more than surface-level wiping; it involves:
- Pathogen Eradication: Using EPA-approved, hospital-grade disinfectants.
- Bloodborne Pathogen Training: Ensuring staff are trained to handle biohazardous materials safely according to OSHA standards.
- Air Quality Management: Utilizing HEPA-filtration vacuums to capture microscopic particles and allergens.
- Documentation: Keeping precise logs of cleaning frequencies and chemical dwell times for compliance audits.
Technical Frameworks of Infection Control in Clinical Settings
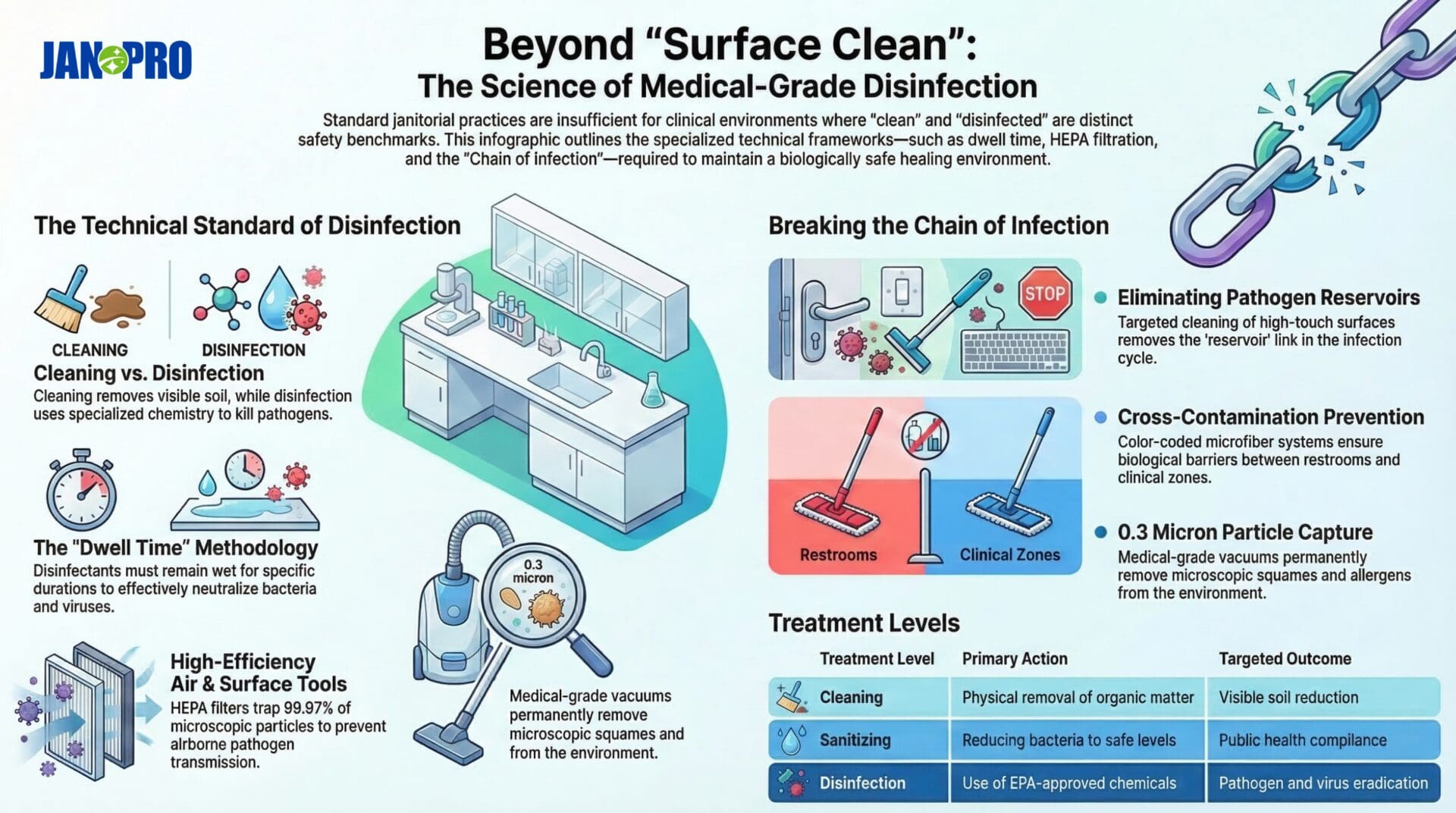
To understand the necessity of specialized sanitation, one must examine the distinction between cleaning, sanitizing, and disinfecting. While cleaning removes visible soil and organic matter, disinfection involves the use of specialized chemicals to kill bacteria and viruses on surfaces.
For a medical facility in the Tampa Bay area, the humidity levels can often influence the persistence of certain pathogens, making the selection of appropriate disinfectants critical.
In high-stakes environments, professionals utilize a “dwell time” methodology. This refers to the specific amount of time a liquid disinfectant must remain wet on a surface to effectively neutralize the targeted pathogens. If a surface is wiped dry too quickly, the chemical reaction may be incomplete, leaving behind viable colonies of bacteria.
Breaking the Chain of Infection
The primary goal of environmental services (EVS) in healthcare is to break the “Chain of Infection.” This cycle consists of six links: the infectious agent, the reservoir, the portal of exit, the mode of transmission, the portal of entry, and the susceptible host.
- Infectious Agent: The pathogen (bacteria, virus, fungi).
- Reservoir: Where the pathogen lives (often high-touch surfaces like bed rails or door handles).
- Mode of Transmission: How the pathogen moves (frequently via the hands of healthcare workers or contaminated equipment).
By maintaining a rigorous schedule for medical cleaning services in St. Petersburg, facilities effectively remove the “reservoir” and “mode of transmission” links, significantly lowering the risk of patient-to-patient spread.
Specialized Protocols for High-Risk Environments
Different areas within a healthcare facility require varying levels of disinfection. While a reception area may focus on high-volume floor care and upholstery, an operating room or diagnostic suite demands terminal cleaning. This process involves the total disinfection of a room between patients, focusing on every surface from ceiling to floor.
Effective sanitation prioritizes the prevention of cross-contamination by employing color-coded microfiber systems. This methodology ensures that tools used in restrooms are never introduced into clinical zones, maintaining a biological barrier between different sections of the facility.
Advanced Surface Materials and Chemical Compatibility
A sophisticated technical aspect of modern medical cleaning is the interaction between disinfectants and the diverse materials found in contemporary clinics. Not all chemicals are suitable for all surfaces. For example, high concentrations of bleach can degrade medical-grade plastics or corrode sensitive electronic diagnostic equipment.
Professional providers must assess:
- Non-Porous Surfaces: Metals, plastics, and glass that require specific surfactants to lift biofilm.
- Porous Surfaces: Upholstery and privacy curtains that may require steam or specialized laundering to achieve deep sanitation.
- Sensitive Electronics: Touchscreens and monitoring devices that require alcohol-based wipes or specialized electrostatic applications to prevent moisture damage to internal circuitry.
The Evolution of Green Cleaning in Healthcare
There is a growing body of research regarding the impact of harsh chemical residues on patient recovery times. Many facilities are now transitioning toward green cleaning protocols. These methods utilize EPA-certified “Design for the Environment” products that offer the same efficacy as traditional chemicals but without the toxic off-gassing.
Using green technologies reduces the presence of Volatile Organic Compounds (VOCs), which is particularly beneficial for pediatric clinics and respiratory therapy centers where patients may have heightened sensitivities.
This approach aligns with the “Healing Environment” philosophy, which suggests that the physical state of a facility—including its air quality and lack of chemical odors—directly influences the speed of patient recovery.
Challenges of High-Traffic Medical Office Buildings
Medical Office Buildings (MOBs) present a unique challenge compared to hospitals. While hospitals have dedicated EVS staff, MOBs often house multiple independent practices—ranging from oncology to podiatry—under one roof. This creates a high volume of traffic in shared elevators, lobbies, and restrooms.
Effective janitorial services in Largo and the surrounding areas must account for these communal “hot zones.” A failure to disinfect a shared elevator button or a check-in kiosk can lead to a facility-wide outbreak. A centralized, data-driven cleaning plan ensures that these transition points are addressed with the same frequency and rigor as the clinical exam rooms themselves.
HEPA Filtration and Indoor Air Quality (IAQ)
While surface disinfection is paramount, the air itself can act as a carrier for pathogens. Dust and skin cells (squames) can harbor bacteria and travel through HVAC systems. Professional medical cleaners utilize vacuums equipped with High-Efficiency Particulate Air (HEPA) filters.
These filters are capable of trapping 99.97% of particles that are 0.3 microns in diameter. In a medical context, this means that during the cleaning process, dust and allergens are not simply kicked back into the air but are permanently removed from the environment. This is a critical component of the methodology used by JAN-PRO Cleaning & Disinfecting in Tampa Bay, ensuring that the environment is safe for both patients and staff.
JAN-PRO: A Standard for Medical Cleaning in Tampa Bay
For healthcare providers in the region, JAN-PRO Cleaning & Disinfecting in Tampa Bay serves as a benchmark for excellence. Through the MedMetrix program, each cleaning professional is trained to handle the specific rigors of medical environments, ensuring that clinics are not just visually clean but biologically safe.
Whether your facility is in need of daily maintenance or specialized terminal cleaning, the team at JAN-PRO is equipped with the technology and certification to deliver results. To discuss a custom-tailored cleaning plan for your facility, contact the regional office at (813) 864-1940 or visit the Tampa location at 6908 W. Linebaugh Ave., Tampa.
About the Author
 Laura Ricchino
Laura Ricchino
Laura Ricchino is Regional Director at JAN-PRO Cleaning Systems of Tampa, based in Florida. She supports operational excellence and growth across the commercial cleaning sector. With a focus on leadership, consistency, and client satisfaction, she works closely with teams to ensure high service standards and strong performance throughout the Tampa Bay region.


 Laura Ricchino
Laura Ricchino